Stebbins sees another outbreak of 18 COVID-19 cases
Last Tuesday, October 6, twelve residents of Stebbins tested positive for COVID-19, sparking fears of another major spike in cases on the scale of the Gambell outbreak that started a few weeks ago. So far, case numbers have stayed lower than in Gambell, but Stebbins is still on high alert.
In addition to the 12 cases announced last Tuesday, two more Stebbins residents tested positive on Friday, October 9, and one positive case appeared on Sunday, October 11, and another three showed up on Tuesday, October 13, bringing the total for this outbreak to 18.
Including the most recent spike, Stebbins has had a total of 23 confirmed cases.
Four of the five previous cases were connected to a cluster with about 30 close contacts, although only three of those contacts are confirmed to have tested positive, and the potential outbreak was contained.
NSHC Medical Director Dr. Mark Peterson said that the newest outbreak is likely unrelated to any previous cases in Stebbins, but is instead tied to a resident flying in from outside the region. “As we see in many of these cases, there appears to be a travel-related source,” he said. “And that’s almost always what we’ve seen, it comes in from the outside.”
Dr. Peterson estimated that there are about 50 close contacts associated with the Stebbins outbreak, significantly fewer than the 200 contacts estimated in Gambell. That may explain why fewer positive cases have cropped up since the initial 12.
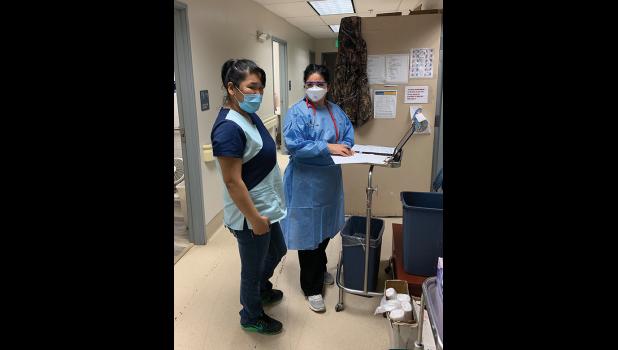
Soon after the first 12 cases were discovered, NSHC sent out a response team with two additional rapid analyzer machines. The team is made up of a physician, a pharmacist and a physician’s assistant, and they work with the clinic staff to facilitate widespread testing while also keeping all the normal clinic operations up and running.
“The backbone of the response team is the clinical team that’s already here,” said Mark Hayward, the physician’s assistant sent along to help with the response. He emphasized that the brunt of the work was being handled by health aides, clinic travel coordinators and patient drivers who live in Stebbins full-time. Their knowledge of the community and tireless dedication to it, he said, has helped keep case numbers low. The team has already tested almost all the known close contacts, as well as about 50 percent of all village residents. They aim to get at least 60 to 70 percent of the village in for testing, an unheard-of fraction in most larger communities around the country.
Stebbins leadership has issued an order to “hunker down” order according to Dr. Peterson, asking people to stay inside their homes and refrain from visiting other households. Shelley Pete, manager of the Stebbins Native Store and Stebbins resident, said people have mostly been following the order. “They’ve been taking extra precautions, and I’ve seen less people out every day,” she said. Those precautions have included a limit to five people in the store at one time, using hand sanitizer and mandatory mask wearing for store visitors.
The Stebbins IRA has been handing out cloth masks, Pete said, and the road to St. Michael has been closed for the duration of the lockdown. She said they expected the lockdown to last at least a month.
Like many villages across the region, Stebbins has very limited housing, which can pose a problem for COVID-19 patients and close contacts needing to isolate and quarantine. So far though, since many of the positive cases were grouped into households that could isolate together, most people have been able to isolate at home.
The Head Start building, which has been sectioned off to sleep about 10 people, has also been used by some patients who needed to isolate away from their families. Over the summer, the Alaska National Guard also handed over ownership of the armory building in Stebbins for use as isolation housing, although it hasn’t been fully converted into housing space yet.
Some people have chafed at the increased restrictions, Pete said, but for the most part people have been cooperating. They’re used to some of the lockdown procedures when there was an uptick in cases in early September, she said, and they’re committed to helping their community get through this challenging time.
Hayward said that personal connections between community members has not only helped slow the spread, but has been an integral part of the successful response. Health aides that are already closely connected to community members are able to mobilize containment and response far faster than the high-tech systems used in bigger cities, he said. He recalled the latest positive case as an example. Last Sunday, a patient tested positive during a routine screening, surprising the clinic staff.
“This happened in the afternoon, and within 15 minutes the health aides who were in the clinic had put together on the back of a sheet of scrap paper the known and likely contacts of that patient,” he said.
While a positive case elsewhere in country would spark a cascade of phone calls and interviews that can take days to complete, health aides in Stebbins were able to get in touch with all of the patient’s close contacts and get them tested in just two and a half hours. Having been part of the Stebbins community all their lives, the health aides knew not only people’s phone numbers, but where they lived, who they lived with, and where they might be able to find them. When they couldn’t get in touch with a potential contact over the phone, they put on their PPE and found them out and about in the community, getting them tested and set up in quarantine before they could potentially spread the virus to anyone else.
Hayward said that rapid response – remarkably faster than elsewhere in the country – was only made possible by the close-knit nature of village life and the dedication of clinic staff.“This is a triumph of human skills over complex hardware and technology,” he said. “I can’t say enough good things about the health aides and their role in community health during this pandemic.”
Funding for this coverage provided in part by a grant from the Alaska Center for Excellence in Journalism.